Disclaimer: This article is for educational purposes only. If you have a foot injury, get it evaluated by a qualified medical professional before attempting any treatment.
You know the feeling. You wake up in the morning, put your feet on the floor, and immediately wince. It feels like someone spent the night stabbing the bottom of your foot. Then it slowly eases up as you move around — only to come roaring back after your next run.
That is plantar fasciitis. It is one of the most common and most frustrating running injuries out there — not because it is severe, but because it lingers for months when you treat only the symptoms instead of the cause.
Here is what is actually going on, and more importantly, how to fix it for good.
What Plantar Fasciitis Actually Is
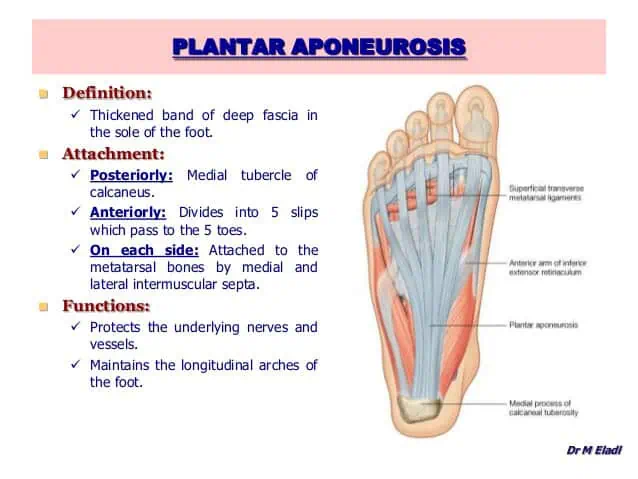
The plantar fascia (plantar aponeurosis) is a thick band of connective tissue that runs along the bottom of your foot, connecting your heel bone to your toes. It supports the arch of your foot and absorbs the impact forces of every step.
When that tissue is chronically overloaded — from too much running, too fast a transition to minimal shoes, poor mechanics, or weak supporting structures — it becomes inflamed and painful. The pain is typically worst first thing in the morning because the fascia tightens overnight and gets rudely reloaded the moment you step out of bed.
The tissue warms up and the pain usually decreases after you have been moving for a while — which makes it tempting to just push through. The problem is that without addressing the root cause, the inflammation never fully resolves and the cycle repeats indefinitely.
Who Gets It and Why
Runners are the most common victims. Every running stride absorbs more than 2.5 times your bodyweight through each foot, at a rate of roughly 330 foot strikes per quarter mile. The cumulative stress adds up extremely fast.
Ruckers face a similar problem. The added load plus the heel-to-toe walking pattern puts sustained stress on the plantar fascia over miles and hours.
Athletes transitioning to minimalist shoes frequently encounter this. Minimalist footwear is not inherently bad — in fact it tends to improve mechanics over time — but the transition needs to happen over months, not days. The foot and calf complex needs time to build the strength and mobility to handle the reduced cushioning.
Anyone who significantly increases activity volume can trigger it. If your training load jumps faster than your tissue’s capacity to adapt, you will overload the system.
The common thread: too much stress, too fast, on tissue that is not prepared to handle it.
The Root Cause Most People Miss
Treating plantar fasciitis with ice, ibuprofen, or rest will reduce the symptoms temporarily. But unless you fix what caused the overloading in the first place, it will come back.
The two most common underlying causes:
1. Tight calves and limited ankle mobility. When the calf and Achilles are tight, the ankle cannot move through its full range of motion efficiently during the push-off phase of running or walking. The foot compensates by rolling inward — which dumps excessive load onto the plantar fascia with every step.
2. Weak glutes and hip external rotators. When the glutes are not doing their job, the knee tracks inward, the arch collapses medially, and the entire load chain shifts in a way that overloads the foot. This is also the root cause of many cases of shin splints — the same movement dysfunction showing up further down the chain.
If you address only the foot and ignore the calf, ankle, hip, and glute function, you are treating the symptom, not the system.
Fix It: Mobility First
Start with the tissue above and below the problem area — calves, ankles, and feet — before adding strength work.
Standing Calf Stretch (Straight and Bent Leg)
The straight leg version targets the upper calf and hamstring. The bent leg version shifts the stretch down into the Achilles and heel. Do both. Spend at least 2 minutes in each position on each leg.
Cossack Squat
One of the best lower body mobility movements available. Keep both feet planted throughout the movement — do not let your heel come up. Start with 5–10 reps each direction, working toward holding the bottom position for a few seconds each rep.
The 10-Minute Squat Hold
Simple, revealing, and uncomfortable if your mobility is limited. Get into a full squat — ass to grass — and just stay there for a cumulative 10 minutes. It will immediately show you where you are tight and need work.
Fix It: Soft Tissue Work
Stretching addresses length. Soft tissue mobilization addresses quality — getting the fascia and surrounding tissues sliding and gliding properly instead of locked down.
Grab a lacrosse ball and spend time mashing your feet, ankles, and calves. Dr. Kelly Starrett’s Mobility WOD has the definitive video resources for this:
Plantar Fasciitis — Kelly Starrett:
Heel and Calcaneus Mobilization:
Fix It: Strengthen the Foundation
Mobility without strength is incomplete. Once you can move better, you need to load the pattern correctly.
Strengthen your glutes. Squats, step-ups, hip thrusts, single-leg deadlifts, and lunges all address the glute weakness that allows arch collapse. If you notice your arch collapsing or your knee caving inward during these movements, reduce the load and focus on maintaining the arch through the full range of motion. Shoes off if possible — direct feedback.
Add barefoot jump rope to your warm-up. Five minutes of continuous barefoot jumping conditions the foot, calf, and ankle complex in a low-load, high-repetition way that transfers directly to running mechanics. It is harder than it sounds and more effective than most foot strengthening exercises.
The bottom line on strengthening: a solid strength and conditioning program that includes heavy compound lower body work will do more to prevent and resolve plantar fasciitis long-term than any amount of foot-specific rehab work in isolation.
The Running Side of the Fix
Plantar fasciitis is frequently a mechanics problem disguised as a foot problem. Heel striking — landing with the foot far in front of the body’s center of mass — creates impact forces that propagate directly through the heel and into the plantar fascia. Improving your running mechanics reduces that loading with every step.
If running-related foot pain is a recurring issue, the Free 5-Part Endurance Mini-Course covers the mechanics and training approach that takes stress off the foot while actually improving your run times. Same method that eliminates most overuse running injuries in the process.
The Summary
Plantar fasciitis is not a foot problem. It is a movement problem that expresses itself in the foot. Fix the movement and the foot heals. Treat only the foot and the problem comes back.
The full fix requires all three pieces working together:
- Mobility — calves, ankles, feet; address the structures above and below the pain
- Soft tissue work — lacrosse ball, aggressive mobilization of the entire lower leg
- Strength — glutes, hips, the arch itself; load the system correctly once you can move correctly
Ice and ibuprofen will calm the symptoms. This will fix the problem.
And once you are back to pain-free running, training smarter with less volume is the long-term insurance policy against this coming back.